Do all types of hepatitis have the same affect on life insurability?
Affordable Life Insurance Policy for Hepatitis A, B and C
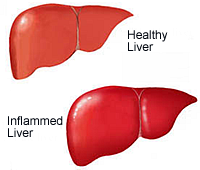
Understanding Different Types of Hepatitis
Hepatitis A, B and C cause varying degrees of liver inflammation. Acute hepatitis can be caused by hepatitis A; chronic hepatitis can be caused by hepatitis B (HBV), hepatitis C (HCV), hepatitis D (HDV), autoimmune diseases such as lupus, various medications, and unknown causes. Learn more on Hepatitis A, Hepatitis B and Hepatitis C.
Other related medical conditions (or medical terminology) include Liver Disease, Liver Cirrhosis, Liver Inflammation, Hep C, Liver Biopsy, Liver Disorders, Seizure Disorder, Viral Load, Acute Hepatitis. Read below for more information on receiving a life insurance quote with these medical conditions.
Hepatitis A
The most common type of hepatitis, as well as the least serious variation of the disease, is hepatitis A. Unlike hepatitis B or C, it will not evolve into a chronic condition. It causes inflammation of the liver; however, it does not usually lead to long-term liver problems and, in most cases, resolves on its own.
This type of hepatitis is contracted after ingesting contaminated food or water or through contact with a person who is currently ill with the disease. The hepatitis A virus is found in the stools of an infected person, or in other bodily secretions, two to seven weeks before symptoms occur and during the first week of illness. It spreads when proper hand cleaning doesn’t occur after bathroom use. It is easily spread at restaurants by employees’ with dirty hands, at day care centers, nursing homes and rehabilitation centers when workers don’t wash their hands properly after changing a diaper or cleaning a patient. People, who eat raw oysters or undercooked clams, as well as travelers visiting a country where hepatitis A is common, are at an increased risk of developing hepatitis A.
Over 85% of people with hepatitis A recover within three months, and over 99% of people recover by six months.
Hepatitis B
Hepatitis B is a virus that is transmitted through blood transfusions, contact with blood in health care settings, through use of contaminated acupuncture needles, tattoo instruments, or shared needles used by drug abusers and during unsafe sex with an infected person. It can be passed from an infected mother to an infant during childbirth.
It takes from one to six months from the time of infection for symptoms of acute hepatitis appear. The risk of becoming chronically infected depends on your age at the time of infection. Most newborns, and about 50% of children infected with hepatitis B, develop chronic hepatitis whereas only a few adults infected with HBV develop the chronic condition.
Most of the damage from the hepatitis B virus is due to the body’s response to the infection. When the body’s immune system detects the infection, it sends out special cells to fight it off, however, these disease-fighting cells can cause liver inflammation. The liver damage also interferes with the body’s ability to get rid of bilirubin which causes jaundice and may progress into a chronic condition.
Hepatitis C
Hepatitis C causes severe liver damage that can lead to deadly health problems. It is spread by infected blood products, shared needles, especially among IV drug users, sexual contact and mother-to-child transmission. Prior to 1992, there was no effective blood screen for the virus and anyone with a blood transfusion prior to that date is at risk. Unlike Hepatitis A or B, there is no preventative vaccine for this disease. People who may be at risk for hepatitis C include long-term kidney dialysis patients, healthcare workers, persons who practice unprotected sex or who use injectible street drugs or individuals who share personal items such as toothbrushes or razors with someone who has the disease.
Although its impact may take decades to become serious, approximately 80 percent of affected individuals with untreated hepatitis C develop chronic inflammation of the liver and severe liver disease. Of those, 10 – 20 percent will develop cirrhosis, a chronic progressive disease that causes scar tissue in the liver, and one to five percent will develop liver cancer.
Identifying Symptoms and Treating Hepatitis
Symptoms of hepatitis do not always present themselves immediately. In acute cases, symptoms of hepatitis A and B are similar to the flu, last for about two months and may include fatigue, nausea, and loss of appetite, unintended weight loss, stomach pain, fever and sore muscles. The skin and eyes may become jaundiced, or yellow, due to the liver’s inability to filter the chemical bilirubin, a breakdown product of old red blood cells in the body. Older individuals may also produce dark urine and clay-colored stools. People infected with hepatitis C are often asymptomatic for many years until the liver develops cirrhosis. Symptoms then are similar to hepatitis A and B, but may also include pain in the upper right quadrant of the abdomen, ascites (fluid in the abdominal cavity), bleeding varices (dilated veins in the esophagus) and generalized itching.
Hepatitis is often found during blood tests for a routine physical or other medical procedure. If, due to symptoms, hepatitis is suspected, a doctor will perform a physical examination to see the liver appears enlarged or tender. Lab work will be ordered to screen for hepatitis antibodies IgM and IgG, elevated liver enzymes, low albumin levels and increased prothrombin time. A liver biopsy may be ordered.
Once the type of hepatitis is identified, a treatment plan will be developed. As there is no specific treatment for hepatitis A, rest is recommended during the acute phase of the disease when the symptoms are most severe. People with acute hepatitis are advised to avoid alcohol and any substances that are toxic to the liver, including acetaminophen (Tylenol). As fatty foods may cause vomiting, because secretions from the liver are needed to digest fats, they should also be avoided. Similarly, hepatitis B warrants no medical treatment other than careful monitoring of liver function through blood tests unless it progresses into chronic hepatitis. Rest may be recommended during the acute phase of the disease when the symptoms are most severe. Those without liver involvement are usually monitored at least yearly to evaluate liver function, detect complications and provide treatment when necessary. Individuals with hepatitis C and chronic hepatitis, who have evidence of liver disease, are sometimes treated with drugs to treat infections and reduce inflammation. Hepatitis C patients are advised to abstain from alcohol, vitamins, nutritional supplements or over-the-counter medications, restrict protein intake and vaccinate against hepatitis A and B infections. There no cure for hepatitis C, but medications in some cases can suppress the virus for a long period of time. Treatment with interferon alpha or a combination of interferon alpha and ribavirin, an antiviral medication, called pegylated interferon alpha, may result in a “sustained response” which means the patient remains free of the hepatitis C virus six months after treatment has been discontinued. This does not mean that the patient is cured, but that the levels of active hepatitis C virus in the body are very low and are probably not causing more or as much damage. On the other end of the spectrum, in cases when liver failure occurs, monitoring in a hospital intensive care unit (ICU) until a liver transplant becomes available may be necessary. A liver transplant is the only cure in cases of liver failure.
How Underwriters View Hepatitis and Insurability
Life insurance underwriters evaluating applications from individuals with a history of hepatitis will want documentation regarding the type of disease (acute or chronic), onset of disease, the absence or presence of symptoms, the results of liver function tests and, some instances, biopsies, as well as an assessment of how a patient has responded to treatment.
Just as there is variation in hepatitis and how it affects an individual’s health in the short term and long run, there is variation in offers of insurance to those affected. Completely resolved cases of acute hepatitis A or B may receive preferred or standard offers even though antigens are present. In chronic hepatitis and hepatitis C cases, underwriters will evaluate the degree of enzyme elevation, stage of liver disease and quality of life, to when rating offers. Although many companies will decline chronic hepatitis C outright, some will consider individuals who have been “cured” for at least two years as documented by negativehepatitis screens.
How Can MEG Financial Help?
At MEG Financial, we have worked with many individuals across the country that have had hepatitis related histories and have helped many obtain fairly priced life insurance. A number of these clients previously attempted to buy life insurance elsewhere but were either turned down or asked to pay a significantly higher rate. Our experience helping others with alcohol related problems is invaluable to you in identifying the insurance company that will treat you most fairly.
For more specific information or to obtain a custom quote, call MEG Financial today at (877) 583-3955. You may also submit this short form and an independent insurance agent will personally contact you to go over any questions or other concerns.

 Speak with an experienced advisor!
Speak with an experienced advisor! 


